[row cols_nr=”2″][col size=”12″]
[/col][/row]
For those who live day to day with pain, life can be difficult. The activities you once took part in may no longer be possible for you because of the pain. The tasks that you need to complete may sometimes have to be put on the back burner until you can gain some form of control over your pain. You may have days where your only focus is on being able to take the edge off of the pain in order to carry on with your life.
As many who suffer with chronic pain already know, there are good days and then there are bad days for chronic pain. When the bad days are really bad, taking the edge off of the pain becomes all that matters.
For those who have pain, there are many avenues that can be traveled to help manage the pain.
Therapies such as physiotherapy, massage and acupuncture with or without medications such as anti-inflammatories, over the counter pain medications, or muscle relaxers are usually the first options to managing pain. If started early enough, the pain can sometimes resolve itself with the help of these non-invasive therapies.
When the pain does not resolve or has become worse, it now reaches a chronic state. At this point, the above therapies can be combined with other interventional treatments to help manage the pain. This includes possible procedures to target the pain source and prescription medications such as muscle relaxers, neuromodulating medications, and opioid pain killers.
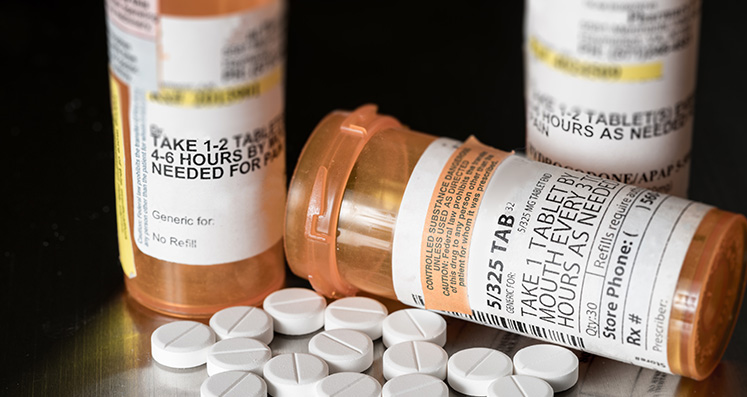
While commonly used to treat acute pain such as pain following a surgery or a broken bone, opioids are also used to manage chronic pain symptoms. While the use of opioids to manage chronic pain has been generally successful, recent studies now provide evidence that shows that the long term use opioid medications can actually be making pain symptoms worse.
Besides the increased risk of dependency and overdose, the increased risk of depression and other mood disorders, and the risk of constipation, recent studies have shown that higher doses and long-term use of opioids may be linked to an increase in pain sensitivity, otherwise known as hyperalgesia. Hyperalgesia is caused by the body’s natural pain tolerance being decreased by chronic opioid use. Our body is equipped with natural painkillers that are released as needed. These natural pain killers consist of chemicals and endorphins. These chemicals and endorphins are made less sensitive by the opioids and therefore, become less effective, making the body more sensitive to pain than they would normally be. This can make the already existing pain much worse.
There is a theory that a percentage of those who have chronic pain and have been on opioids long-term are not experiencing pain from the original injury, but rather they are experiencing amplified pain due to the opioids they are taking.
Dr. Erin Krebs, medical director of Women’s Veterans Comprehensive Health Care System took a deeper look into this theory by examining 67 other studies on effects of a decrease in opioid medications on pain patients who had been taking opioids long-term. She found that many of the studies showed that over time, there was a decrease in pain level, as well as an increase in mobility and an overall improvement in quality of life. The most successful programs were those that offered a multidisciplinary approach to pain management and incorporated psychological treatments, physical treatments, interventional treatment, nutrition education and rehabilitation.
That being said, there are those who do get great benefit from opioid use for chronic pain symptoms. When the dosage of opioids is low and consistent, and the individual is coupling their medication with other interdisciplinary treatments to increase mobility, long –term opioid use can pose less of a risk to the patient. However even those patients should be monitored closely by their primary care physician, and keep an opened mind should their physician want to discuss slowly tapering down on their medications.
Attempting to decrease or come off of an opioid medication should not be done on impulse and it should never be done alone. A physician should always be made aware of your decision to decrease your medications. Physicians are trained in the slow tapering off of opioid medications, as well as the various warning signs of withdrawal. Decreasing your opioid medications should be a team effort between you and your primary care physician. Opioid withdrawal is a very real occurrence that can be slow, sickening, painful and even deadly. For this reason, your primary care physician should always be included in all concerns or questions regarding your opioid medications. A slow and medically supervised decrease in dose is the ideal way to taper off of opioids. Any other way can have serious consequences.
Talk to your primary care physician about your options when it comes to your opioid medications. All prescriptions should be taken exactly as your physician has prescribed it to avoid physical harm.


